Societal Issues
Incidental Findings:
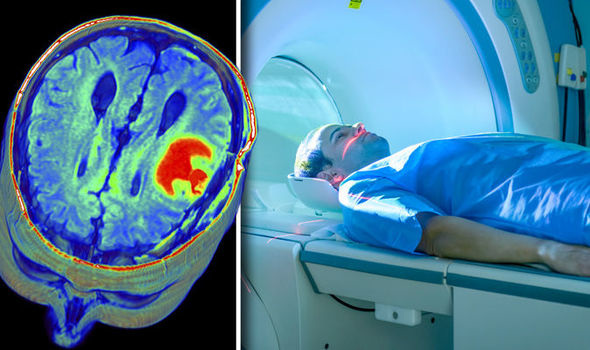
One societal issue lies in the controversy when "incidental findings" are found during these scans when used for research or diagnosis purposes. An incidental finding is "a finding concerning an individual research participant that has potential health or reproductive importance and is discovered in the course of conducting research but is beyond the aims of the study" (Nelson 2008). The main issue revolves on whether the researchers should disclose these incidental findings to the volunteer of a study or a physician for a better diagnosis. Researchers are not doctors and are not responsible for reporting it. Some believe its better to not reveal these findings in order to stop volunteers from worrying and others believe that they should have a right to know whether it is serious or not.
In addition, in the medical field, there are many issues about determining whether the incident finding is real or merely a false alarm or if they can be found at all.
The reasons behind this uncertainty include:
One societal issue lies in the controversy when "incidental findings" are found during these scans when used for research or diagnosis purposes. An incidental finding is "a finding concerning an individual research participant that has potential health or reproductive importance and is discovered in the course of conducting research but is beyond the aims of the study" (Nelson 2008). The main issue revolves on whether the researchers should disclose these incidental findings to the volunteer of a study or a physician for a better diagnosis. Researchers are not doctors and are not responsible for reporting it. Some believe its better to not reveal these findings in order to stop volunteers from worrying and others believe that they should have a right to know whether it is serious or not.
In addition, in the medical field, there are many issues about determining whether the incident finding is real or merely a false alarm or if they can be found at all.
The reasons behind this uncertainty include:
- There is a rapid increase of higher-field scanners; for example, 3 Tesla scanners have, in many places, replaced 1.5 Tesla scanners, and 4 and 7 Tesla scanners are now much more common than they once were in the past (Nelson 2008). With higher field strength come greater sensitivity. Therefore, there is a greater likelihood of false positives (false incident findings) and detecting a problem when one doesn't actually exist.
- As the use of MRI continues to increase quickly, and the number of scans being performed increases, it is difficult to predict what the true rate of Incident findings will be to determine whether they are true or false.
- The cost involved in having a neuroradiologist read a scan is large, therefore there is a financial disadvantage to having such experts read each scan.
Safety Of MRIs:
With the great number of benefits to this procedure, there are still a few worries regarding the safety of patients during an MRI scan. The powerful magnetic field of the MR system can attract iron-containing (ferromagnetic) objects and may cause them to move suddenly with a great force. This poses as a possible risk to the patient or anyone in the object's "flight path." Great care is taken to be certain that objects such as ferromagnetic screwdrivers and oxygen tanks are not brought into the MR system area. There have been accidents where patients have been injured due to the close proximity of a magnet object too close to the MRI becoming attracted to the MRI's magnetic force. In addtion, the magnetic field of the MR system may damage external hearing aids or cause heart pacemakers, electrical stimulators, or neurostimulators to malfunction or cause patient injury. If there are any other metallic fragment in the patient's body there is a potential risk that it could change position and possibly cause an injury to the individual internally. Also, a metallic implant or other object may cause signal loss or distort the MR images which can leading to a wrong diagnosis and incidental findings.
With the great number of benefits to this procedure, there are still a few worries regarding the safety of patients during an MRI scan. The powerful magnetic field of the MR system can attract iron-containing (ferromagnetic) objects and may cause them to move suddenly with a great force. This poses as a possible risk to the patient or anyone in the object's "flight path." Great care is taken to be certain that objects such as ferromagnetic screwdrivers and oxygen tanks are not brought into the MR system area. There have been accidents where patients have been injured due to the close proximity of a magnet object too close to the MRI becoming attracted to the MRI's magnetic force. In addtion, the magnetic field of the MR system may damage external hearing aids or cause heart pacemakers, electrical stimulators, or neurostimulators to malfunction or cause patient injury. If there are any other metallic fragment in the patient's body there is a potential risk that it could change position and possibly cause an injury to the individual internally. Also, a metallic implant or other object may cause signal loss or distort the MR images which can leading to a wrong diagnosis and incidental findings.
Future Societal Issues
There are issues regarding whether or not MRIs affect human health when exposed to such powerful magnetic fields. Currently there is concern regarding whether this exposure can lead to long term health effects. Studies into the MRI and the effects of regular exposure to the magnetic fields will be conducted to see if the magnetic fields could raise a risk to cancers or other diseases.
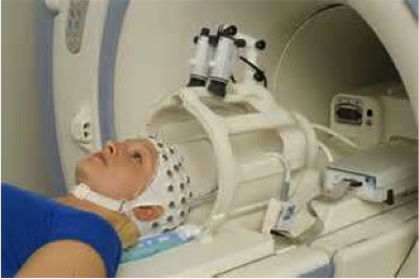
Using MRI technology, an fMRI (functional magnetic resonance imaging) can prove to have applications in lie detection. An fMRI measures and examines the activity in the brain. Three courts in the U.S have admitted the use of fMRI lie detection as evidence in their case. In multiple studies, blood oxygen dependent activity was measured when the subject was told to lie. The areas in the brain associated with deception were studied for activity. The results revealed that the "lie" trials associated more with brain activity than the "truth" trials. The question of concern is how accurate are these results? Different factors associating with cognitive, personality and the brain may affect the validity of this study. Age, psychiatric conditions, and individual traits decrease the applicability of these tests concerning these individuals as they have not been validated in these populations.
As of August 18, 2015, a recent medical breakthrough has shown that the MRI can provide more than images, it can actually be used to treat cancer. Cells that have been injected with a iron oxide nanoparticles are steered by MRI scanners to to both primary and secondary tumour sites within the body. Testing on mice has proven that this method works, however it will be many more years of research to confirm.
Using MRI technology, an fMRI (functional magnetic resonance imaging) can prove to have applications in lie detection. An fMRI measures and examines the activity in the brain. Three courts in the U.S have admitted the use of fMRI lie detection as evidence in their case. In multiple studies, blood oxygen dependent activity was measured when the subject was told to lie. The areas in the brain associated with deception were studied for activity. The results revealed that the "lie" trials associated more with brain activity than the "truth" trials. The question of concern is how accurate are these results? Different factors associating with cognitive, personality and the brain may affect the validity of this study. Age, psychiatric conditions, and individual traits decrease the applicability of these tests concerning these individuals as they have not been validated in these populations.
As of August 18, 2015, a recent medical breakthrough has shown that the MRI can provide more than images, it can actually be used to treat cancer. Cells that have been injected with a iron oxide nanoparticles are steered by MRI scanners to to both primary and secondary tumour sites within the body. Testing on mice has proven that this method works, however it will be many more years of research to confirm.
|
|
Future of fMRI Functional MR imaging provides information that can be used in planning therapy of or the surgical approach to brain tumors. MRIs study brain anatomy where as Functional MRI is used to study brain functions. This form of MRI reveals what parts of the brain are active when thinking of certain things. Different parts of brain light up depending on different items, using this patients who are considered brain dead or those who can't communicate in any other way are placed in here so that physicians can diagnose their patients through their MRI scans.
How it works: The patient is asked to perform a simple task such as miving their fingers for a short time while multiple echo-planar images of the motor cortex are done. The subject discontinues the task for a short period while imaging continues. Task-on and task-off imaging is performed several time. The compiled data is then processed to generate a map of the regions in the brain that reveals repeatedly increased or decreased blood oxygen levels. *Echo-planar imaging make it possible to obtain individual MR slices in the time frame of 50-100 msec, thus shortening the time of MR imaging. |
"Overuse" Of Medical Imaging
With the increase in medical imaging technologies also increases our reliance on these machines. Conflicting reports have emerged about whether these additional tests are having a positive impact on diagnosis—and cure—rates. A new study shows that for life-threatening injuries, a threefold increase in the number of computed tomography (CT) and magnetic resonance imaging (MRI) scans in emergency rooms has not resulted in an improvement in useful diagnosis (Harmon 2010).
Researchers found that in 1998 a person admitted to an emergency department with an injury had about a 6% chance of having a CT or MRI scan. In 2007 that number rose to 15%. Life-threatening conditions were uncovered by these scans in 1.7 percent of the sampled 1998 ER visits and about two percent of those sampled in 2007. The most dramatic usage increase occurred between 2003- 2007, during which time the percentage of injured patients who received CT/ MRI scans almost doubled (Harmon 2010).
Doctors face a dilemma regarding the number of tests being done on so many. Not every person requires a test, but doctors fear that if tests aren't done, they may miss something vital to the patient's recovery. Some things can't be found with just a physical examination or an x'ray. The miss rate will increase if they decrease the number of tests done. To doctors underdiagnosis is "a significant source of liability" when treating patients.
Physicians' guidelines for deciding when to order scans are already in place, but just how much doctors follow them is fuzzy. In the future more refined scanning technology with lower standard radiation doses, along with decision-support software, might help researchers know what patients are the best candidates for CT or MRI scans—and protect patients who do undergo scanning (Haroman 2010).
With the increase in medical imaging technologies also increases our reliance on these machines. Conflicting reports have emerged about whether these additional tests are having a positive impact on diagnosis—and cure—rates. A new study shows that for life-threatening injuries, a threefold increase in the number of computed tomography (CT) and magnetic resonance imaging (MRI) scans in emergency rooms has not resulted in an improvement in useful diagnosis (Harmon 2010).
Researchers found that in 1998 a person admitted to an emergency department with an injury had about a 6% chance of having a CT or MRI scan. In 2007 that number rose to 15%. Life-threatening conditions were uncovered by these scans in 1.7 percent of the sampled 1998 ER visits and about two percent of those sampled in 2007. The most dramatic usage increase occurred between 2003- 2007, during which time the percentage of injured patients who received CT/ MRI scans almost doubled (Harmon 2010).
Doctors face a dilemma regarding the number of tests being done on so many. Not every person requires a test, but doctors fear that if tests aren't done, they may miss something vital to the patient's recovery. Some things can't be found with just a physical examination or an x'ray. The miss rate will increase if they decrease the number of tests done. To doctors underdiagnosis is "a significant source of liability" when treating patients.
Physicians' guidelines for deciding when to order scans are already in place, but just how much doctors follow them is fuzzy. In the future more refined scanning technology with lower standard radiation doses, along with decision-support software, might help researchers know what patients are the best candidates for CT or MRI scans—and protect patients who do undergo scanning (Haroman 2010).